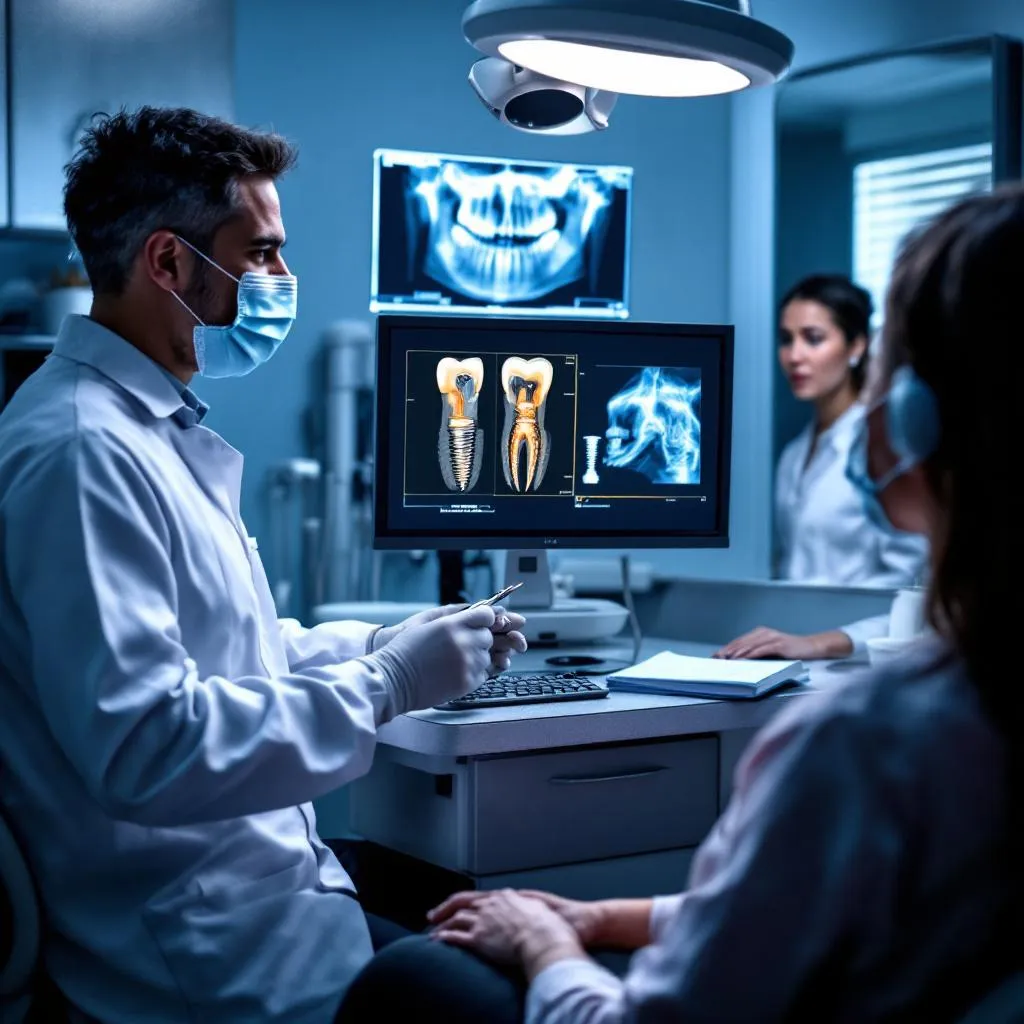
As a dental implants expert practicing in North Hollywood, I often meet patients who are worried about complications after they’ve chosen Dental Implants. In this area, people expect reliable, long-lasting solutions for missing teeth, and it’s important to understand the common issues that can arise, how to spot them early, and what to expect from the treatment process. My goal in this article is to walk you through practical explanations and real-world advice so you feel confident about your care.
Dental Implants: Common Causes of Problems
Dental implants are a predictable treatment, but like any medical procedure they carry risks. Problems usually start with the interface between the implant and the bone or the gum. Failure of osseointegration, which means the implant does not properly fuse with the jawbone, remains a leading cause of early failure. This can be influenced by factors such as smoking, uncontrolled diabetes, poor bone quality, and infection at the surgical site. Later issues often relate to mechanical complications like loose components, fractures of the prosthetic crown or abutment, and wear on the surrounding natural teeth.
Recognizing Infection and Peri-Implantitis
One of the most concerning complications I see is peri-implantitis, an inflammatory condition that affects the tissues around the implant and can lead to bone loss. Early signs include redness, swelling, tenderness, and persistent bleeding around the implant. Unlike ordinary gum irritation, peri-implantitis may progress silently before you notice obvious symptoms. Routine follow-up visits allow for early detection; X-rays and probing depths help quantify bone levels and tissue health. When managed early, peri-implantitis can often be treated without losing the implant.
Mechanical Complications and Bite-Related Issues
Not all problems are biological. Mechanical issues can develop over time, particularly when bite forces are not evenly distributed. A single implant that receives too much force may lead to loosening of the abutment screw or fracture of the prosthetic crown. Bruxism, or night grinding, is a common contributor. Proper planning during the restorative phase—choosing the right implant size, angulation, and crown material—reduces the risk. If a mechanical problem does occur, many issues can be resolved with adjustments, tightening, or replacement parts rather than full implant removal.
Bone and Soft Tissue Considerations
Successful implants depend on adequate bone volume and healthy soft tissue. In North Hollywood, patients often present after years of missing teeth with significant bone resorption. Bone grafting and sinus lifts are common adjunctive procedures that create a stable foundation for implants, but these steps also introduce additional healing needs and potential complications. Soft tissue health is equally important; inadequate gum thickness can make the implant appear unaesthetic or more prone to irritation. A careful evaluation of the tissue biotype and appropriate grafting when needed are key to long-term success.
Prevention, Maintenance, and the Role of the Patient
Prevention starts with a thorough pre-surgical evaluation and continues with excellent home care and routine professional maintenance. I emphasize to patients that implants require the same respect as natural teeth: regular brushing, flossing around the implant, and attending scheduled hygiene visits. Smoking cessation and control of systemic conditions like diabetes significantly improve outcomes. If problems arise, prompt intervention—whether it’s a deep cleaning, localized antibiotics, or a restorative repair—can prevent more significant complications.
For patients seeking more information mid-treatment or exploring options, I recommend they consult with a skilled implant team that coordinates surgical and restorative planning. If you are researching reliable resources, our practice provides focused education and tailored treatment plans, and we discuss long-term maintenance strategies to ensure predictable results. In North Hollywood many patients find that understanding possible complications ahead of time reduces anxiety and leads to better cooperation during the healing phase. I also encourage open communication so we can identify and treat issues early, often avoiding more invasive interventions.
When complex complications occur—such as advanced peri-implant bone loss or implant fracture—referral to a specialist or collaborative care with an oral surgeon and prosthodontist may be necessary. Salvage procedures can include surgical debridement with regenerative techniques, implant replacement after site reconstruction, or prosthetic redesign to distribute forces differently. Each case is unique, and I prioritize individualized plans that balance long-term function, aesthetics, and the patient’s goals.
Patient Experience and Recovery Expectations
Most patients can expect a relatively straightforward recovery when implants are placed by an experienced team. Mild discomfort and swelling are common in the first few days and typically managed with over-the-counter pain control and cold compresses. Clear post-operative instructions about oral hygiene, diet, and activity level reduce the incidence of complications. For more complex reconstructions, staged approaches lengthen treatment time but often improve predictability and overall satisfaction.
Frequently Asked Questions
Q: How soon will I know if an implant is failing? A: Early failure often becomes evident within the first few months if an implant fails to integrate; signs include mobility, persistent pain, or infection. Late failures may develop gradually and present with inflammation or changes on X-rays.
Q: Can peri-implantitis be reversed? A: In many cases, early peri-implantitis can be managed with nonsurgical cleaning and localized therapies. Advanced cases may require surgical intervention and regenerative techniques to restore lost bone.
Q: Are implants painful to place? A: Most patients tolerate the procedure well with local anesthesia and, when needed, conscious sedation. Post-operative discomfort is typically mild and short-lived.
Q: How long do implants last? A: With proper care and maintenance, implants can last decades. Factors such as oral hygiene, systemic health, and habits like smoking influence longevity.
Q: What if I grind my teeth? A: Bruxism increases the risk of mechanical complications. We often recommend nightguards and occlusal adjustments to protect implants and restorations.
If you’re in North Hollywood and thinking about restorative options, I’m happy to discuss how we minimize risk and tailor treatment to your situation. Whether you’re preparing for surgery or managing a current concern, clear communication and timely care are the cornerstones of successful outcomes.
To learn more about the procedure, what to expect during recovery, and how we handle complications, contact our office. We’re committed to helping you achieve durable, natural-looking results with Dental Implants in a comfortable, patient-centered environment, and we’ll develop a treatment plan that fits your needs.
Ready to take the next step? Reach out to schedule a consultation so we can evaluate your oral health, discuss restorative options, and design a maintenance program that protects your investment in Dental Implants. Our team provides compassionate care and clear guidance at every stage of treatment.
Dr. Ahdout
11126 Chandler Blvd, North Hollywood, CA 91601, United States
Phone: Find us on Google Maps